Framework of oppression, and problems of ‘mental health’ and stigma talk
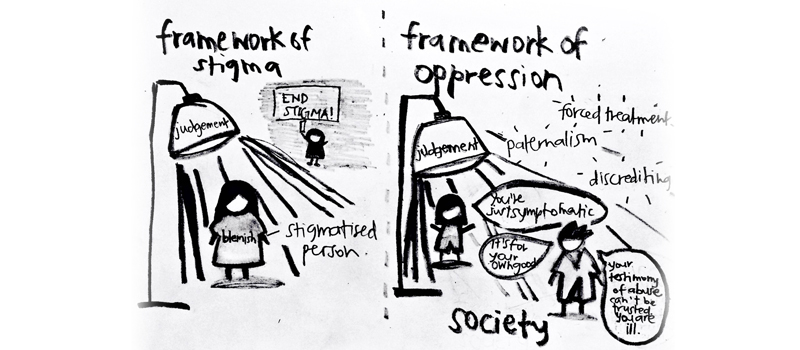
An argument to reframe the discussion in terms of oppression of users and survivors of psychiatry, to acknowledge psychiatric oppression, and to recognise that madness is not a personal tragedy but the outcome of social organisation.By Emmy CharissaLast Monday was World Mental Health Day. I am someone who would be classified as having a ‘mental health problem’, but I do not like World Mental Health Day and it is not relevant to me. I have experienced low moods and anxiety for more than twenty years, and probably never will be ‘mentally healthy’. Further, I think there are many problems with talking about ‘mental health’, ‘stigma’ and ‘recovery’, three ideas that have received a lot of attention over the past week. Let me tell you why.World Mental Health Day centres the ‘mentally healthy’ World Mental Health Day is as much about people who live with long-term mental illnesses as a World Hearing Day would be about peoples who are Deaf or Hard of Hearing, or a World Health Day would be about people who live with chronic illnesses.Under a framework of ‘mental health’, people who have extreme mood states, who hear voices, who have altered states of consciousness, or who have other non-normative psychological experiences commonly labelled as ‘mental illnesses’ are viewed as deviant, if only as a deviation from the norm of the ‘mentally healthy’.And while advocates might try to reduce the stigma of ‘mental health problems’ or ‘mental illnesses’, the inclusion of the words ‘illness’ and even ‘health’ still foregrounds the idea that people with ‘mental health problems’ are defective in some way.There are a variety of better terms out there to describe us and our experiences. We are users and survivors of psychiatry, the term used by one of the international user/survivor groups which played a key role in the drafting of the Convention on the Rights of Persons with Disabilities; people with psychiatric or psychosocial disabilities, the term used by the United Nations, and so on. There is also the reclaimed term “madness”, which avoids medicalising non-normative psychological experiences, and which has been adopted by the emerging field of mad studies.The problem with ‘mental health’ talkFurther, the discourse of ‘mental health and illness’ places the responsibility on the ‘mentally ill’ to try and normalise themselves by becoming ‘healthy’. Many people with who have been diagnosed with mental illnesses do want to feel better, and many advocates who partake in mental health talk do not think the responsibility to ‘reintegrate’ lies solely in the individual with the mental illness. However, the framework of mental health itself pushes this idea and in the process individualises social problems.In fact, many of the barriers that people who have been diagnosed with mental illnesses face reside in society – discrimination at the interpersonal and institutional levels; paternalising and discrediting people who have been diagnosed or labelled; and economic practices that are built around the idea of a ‘healthy’ nondisabled person.Not recovery and resilience, but possible ways of livingIt is for these reasons that I take issue with the focus on ‘recovery’ and ‘resilience’ in the current discourse, since these concepts can be used to individualise what are really social problems. Resilience, moreover, comes with moral connotations. A much better way to talk about it, I think, is to talk about possible ways of living.Hence, holding down a regular job may be impossible for someone, but this does not mean that the person is not ‘resilient’ or has not ‘recovered’. It simply means that we as a society need to create a world where it is possible for people to live lives not fraught with financial struggle even if they cannot hold down a job. Madness, as disability studies scholars would say, is not a personal tragedy, but a matter of social organisation.I also take issue with the focus on people being able ‘recover and lead productive lives’. While many people who have been diagnosed with mental illnesses do recover, there are those who do not, and we must be careful not to further marginalise other groups in our own advocacy efforts.From a framework of stigma to a framework of oppressionThis bring me to another problem with the current discourse: framing the issue in terms of stigma. There are two related points here.First, talking about the stigma of mental illness constantly refocuses our attention on the deviance and moral blemish frequently associated with mental illness, and the judgement passed on those who have been diagnosed with them. In contrast, oppression focuses on and passes judgement on society and on systems of oppression, and provides the oppressed with a way to call out those who oppress them.Second, framing the problem in terms of stigma isolates, while framing the problem as oppression connects. The latter allows us to target the source of the problem – oppressive cultural beliefs and social practices – and connects us to other oppressed groups, including women, ethnic minorities, stateless peoples, LGBTIQ people, and other groups of disabled peoples.It is so important to be able to name the wrongs that have been perpetrated against oneself. I would like to introduce you to a term you can use for the oppression of people who have been diagnosed or labelled with mental illnesses: disablism. Disablism refers to the oppression of people society constructs as ‘disabled’ – wheelchair users, blind and partially sighted people, Deaf peoples, neurodivergent people, and people who have been diagnosed / labelled with mental illnesses. It is analogous to sexism, racism and the like. This term also has the benefit of holding that people cannot choose between which disabled peoples they discriminate against and which they do not.When treatment hurts and re-traumatisesCampaigns need to go beyond educating the public, since some of the worst forms of oppression happen behind the closed doors of mental health institutions. Such oppression can take the forms of paternalism, infantilisation, and/or degrading treatments, to give some examples, and may be so normalised that they are not even considered as oppressive or even just wrong.One of the ways in which people diagnosed with mental illnesses are oppressed is the way in which they are treated as inpatients in psychiatric wards. There have been many stories, passed amongst friends and within the movement of users and survivors of psychiatry, of being traumatised by the use of force and the loss of dignity experienced in psychiatric wards.Psychiatric wards employ different methods to try and calm or ‘manage’ patients, and not all of them are benign. One distressing practice is the use of restraints, which medical professionals justify as being in the ‘best interests of the patient’ but which many users/survivors experience as traumatic. Restraints are in theory only to be used as a last resort, but in practice are also used for convenience. For people who have lived through violence, the experience of being tied down can be severely re-traumatising, even causing flashbacks of being raped or sexually abused.Yet, there is silence about this in the public sphere. We – users/survivors and allies alike – need to have this conversation, not just one about ‘seeking treatment’. All of us need to pay attention to the voices of those who have survived psychiatry and acknowledge the pain that has been forced on people through the years. We must do so, or those who seek treatment will continue to be hurt just like those of us who have survived psychiatry have been.Fulfilling our obligations under the UN Convention on the Rights of Persons with DisabilitiesSingapore has ratified the United Nations’ Convention on the Rights of Persons with Disabilities (CRPD), a legally binding international human rights treaty. The UN recognises people who have been diagnosed or labelled with mental illnesses as disabled people who are covered by the CRPD, and the CRPD protects us from forced, coerced and/or degrading treatment or punishment. The state now has a legal duty to protect people with psychosocial disabilities from such rights violations, or explain its failure to do so.Users and survivors of psychiatry fought for decades to build alliances with other groups of disabled peoples and to be included in the cross-disability movement, cumulating in having our concerns recognised in the CRPD. Let those of us who have survived psychiatry build on these successes end our silence once and for all.The UN Disability Convention:United Nations Convention on the Rights of Persons with DisabilitiesThe problems with physical and mechanical restraints:Why They Die: Little Training, Poor Staffing Puts Lives at RiskA legal view by prominent law professor Elyn R. Saks in the Yale Law Journal:The Use of Mechanical Restraints in Psychiatric HospitalsEmmy CHARISSA is an anthropology/sociology graduate student who is involved in the feminist and disabled peoples’ movements. A user/survivor of psychiatry, she used to avidly peruse the literature on the stigma of mental illness until she was introduced to disability studies and realised its liberatory potential. She has recently started to explore Deaf studies and the emerging field of mad studies, and is interested in cultural/discursive alternatives and possible ways of living.








